Premenstrual syndrome (PMS) symptoms during perimenopause can mirror those of menopause symptoms, confusing women as to what exactly are they suffering from and what initiatives they should take to find relief.
Continue reading to learn more about PMS and perimenopause, including the causes of their symptoms, how to differentiate between PMS and perimenopause symptoms, and much more.
Causes of PMS and Perimenopause Symptoms
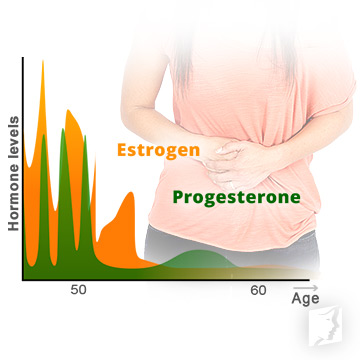
The symptoms of PMS and perimenopause are due to hormonal events in women's lives.
Several theories have taken forefront throughout the years on what causes PMS symptoms, among them being women's sensitivity to hormonal fluctuations of estrogen, progesterone, and serotonin starting mid-cycle and extending into menstruation.
Classic grievances experienced during PMS include:
- Irritability
- Cramps
- Cravings
- Headaches
- Bloating
On the other hand, perimenopause symptoms arise from the decline of aforementioned sex hormone levels with the cessation of ovarian reproductive functions, often beginning with irregular periods as well as other symptoms, including:
How to Differentiate between PMS and Perimenopause Symptoms

Without a doubt, trying to find a difference between PMS and perimenopause symptoms can be a difficult task, even for the most experienced healthcare professionals.
Nevertheless, keeping the aforementioned causes of symptoms in mind, an approach can be applied in attempt to discern between the two.
Women can consider symptoms to be due to PMS if they occur on a cyclical basis during the time leading up to menstruation.
Whereas, symptoms can be attributed to perimenopause if periods are abnormal; women are around the age of menopause (mid 40s or early 50s); and symptoms do not correspond with the time of menstruation.
It has been documented that some women experience severe PMS during perimenopause when the life stage first begins, and menstrual cycles are still regular. They find relief later on as they get closer to menopause, and menstrual cycles become irregular.1 However, this is not a steadfast rule.
How to Address Symptoms

Because both PMS and perimenopause symptoms have hormonal influences, many of the same measures may be pursued for relief, starting with lifestyle changes.
Lifestyle changes that promote optimal endocrine system health include:
- Enriching one's diet with B vitamins, calcium, vitamin D, and other essential nutrients
- Exercising regularly for a mood boost, healthy weight, and better sleep habits
- Practicing stress-relief techniques of yoga, tai chi, meditation, or a favorite hobby
- Controlling addictions to caffeine, alcohol, tobacco, and illicit drugs
Likewise, alternative medicine can be pursued alongside lifestyle adjustments for optimal results, such as:
- Phytoestrogenic herbal supplements, like black cohosh or chasteberry
- Hormone-regulating supplements, like Macafem
Further natural and effective options can be followed as a comprehensive menopause symptoms treatments plan.
However, if PMS and perimenopause symptoms persist after pursuing less risky alternatives, prescription medications may be undertaken (with risks involved). They include:
- Birth control
- Selective serotonin re-uptake inhibitors (SSRIs)
- Hormone replacement therapy (HRT)
In all cases, it is advisable to speak with your doctor to determine the best line of action for your mental and physical health. A combination of approaches may be most effective.
Conclusions
While it is true that PMS symptoms share many of the same woes as perimenopause symptoms, both can be managed and treated successfully for long-term wellness. With a little bit of investigative work and self-awareness, women can tap into their body's cues as to what nourishment it needs to get back on track to optimal health. Relief is only a step away!
Sources
- Hassan, I. et al. (2004). PMS in the perimenopause. The Journal of the British Menopause Society, 10(4), 151-156. doi: 10.1258/1362180042721111
- Mayo Clinic. (2018). Premenstrual syndrome (PMS): Symptoms & causes. Retrieved October 22, 2019, from https://www.mayoclinic.org/diseases-conditions/premenstrual-syndrome/symptoms-causes/syc-20376780
- Society for Endocrinology. (2019). Premenstrual syndrome. Retrieved October 22, 2019, from https://www.yourhormones.info/endocrine-conditions/premenstrual-syndrome/
Footnotes:
- Our Bodies Ourselves. (2011). What to Expect in Perimenopause. Retrieved October 22, 2019, from https://www.ourbodiesourselves.org/book-excerpts/health-article/what-to-expect-perimenopause/

