Did you know?
Testosterone is the hormone responsible for bone strength and breakdown in men.
Bone health is inextricably linked to hormones. For this reason, women make up about 80% of osteoporosis sufferers, and a large percentage of those women have completed the menopause transition and experienced the hormonal fluctuations associated with it. Estrogen is the predominant hormone that fades with the onset of menopause and puts women at a much higher risk of developing osteoporosis.
However, there are other causes of osteoporosis. Continue reading below to learn about the hormonal and other causes of this disease that weakens bones.
Hormonal Causes of Osteoporosis
Although osteoporosis can affect both men and women at any age, up to 80% of osteoporosis sufferers are women. In fact, up to 33% of women over 50 will experience an osteoporotic bone fractures. This is the average age where women begin to experience menopause, which causes hormone fluctuations. Because bones in the female body are heavily dependent on estrogen to regulate the bone growth cycle, women's bones become weak and brittle as their estrogen levels diminish.
Also, because women are more susceptible to osteoporosis, they should better understand this disease and incorporate any possible preventative measures early on.
It's helpful to take a closer look at exactly why low estrogen levels lead to osteoporosis. By better understanding the causes of osteoporosis, women can manage it or even prevent its onset. The information below will describe how estrogen affects bones.
Estrogen and osteoporosis
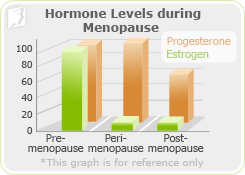
The graph to the right shows how drastically levels of estrogen drop off during menopause and postmenopause, beginning at about age 45. Estrogen levels in postmenopausal women are about one-tenth the levels in premenopausal women. For this reason, women approaching menopause and those who have already gone through it are at a much higher risk of developing osteoporosis and suffering from bone fractures as a result.
Without adequate levels of estrogen, the bones are unable to absorb the proper amounts of calcium to replenish bone mass as cells slough off and die. The body also has trouble controlling the amount of bone cells that are destroyed without estrogen to regulate the function.
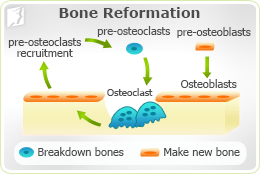
While estrogen has many important functions, one of its most important functions is its prevention of bone breakdown, known as resorption. Healthy bones require a balance of osteoclasts (cells that breakdown bones) and osteoblasts (cells that make new bone). As estrogen levels diminish, osteoclasts live longer than their counterparts, osteoblasts. This leads to bones degenerating at a rate much greater than they can be rebuilt, making them grow weak and brittle.
Another part of estrogen's role in bone reformation involves maintaining normal levels of vitamin D, which is required for absorbing calcium into the bones. As estrogen levels decrease, vitamin D levels follow suit, and bone strength suffers. In addition to hormonal causes of osteoporosis, other factors can drastically diminish bone strength. Continue reading to find out the other causes of osteoporosis.
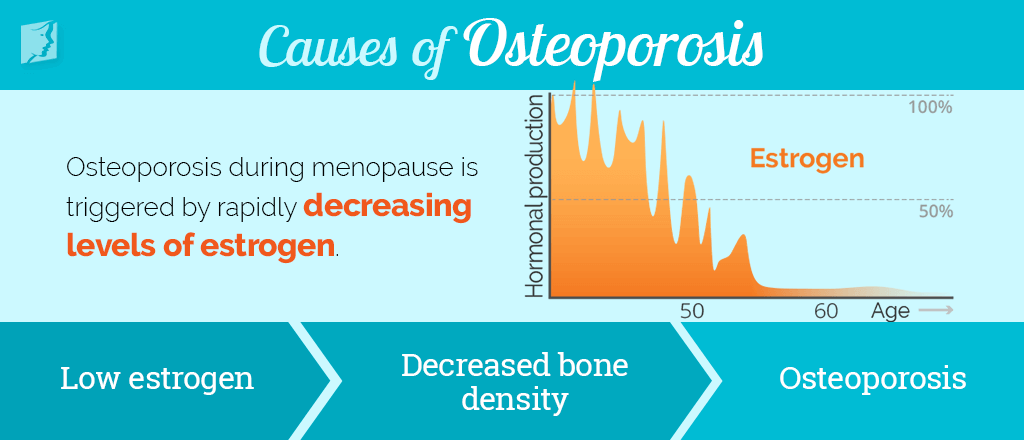
Other Causes of Osteoporosis
The primary cause of osteoporosis in women as they surpass age 50 is diminished hormonal levels, particularly estrogen levels. However, there are other causes that can contribute to the onset of osteoporosis. Other causes of osteoporosis include the following:
Diseases. Many diseases can hamper the growth of new bone material. Some of these diseases are hyperthyroidism, disorders of the adrenal glands (Cushing's syndrome), disorders of the pituitary gland, diabetes, and eating disorders.
Medications. Some medications can reduce the bones' ability to rebuild themselves. Some of the medications that can cause osteoporosis are glucocorticoid medications, prednisolone, excess thyroid hormone replacement, the blood thinner heparin, and certain anticonvulsant medications.
Insufficient bone growth as a youth. Bones that didn't get enough calcium early in life have a higher likelihood of becoming osteoporotic and fracturing as estrogen levels begin to decrease.
- Genetic factors. If a woman's family members, especially her mother, have suffered from osteoporosis, the likelihood that she will develop the disease jumps dramatically. Genetics also help determine the body type of a woman. If she inherited a small, thin body type, she is predisposed to osteoporosis.
Click on the following link to find out about osteoporosis prevention.
Sources
- Christenson, E.S. et al. (2012). Osteoporosis management in post-menopausal women. Minerva Ginecologica, 64(3), 181-194. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/22635014
- Cleveland Clinic. (n.d.). Menopause and Osteoporosis. Retrieved May 10, 2016, from https://my.clevelandclinic.org/health/diseases_conditions/hic-what-is-perimenopause-menopause-postmenopause/hic_Menopause_and_Osteoporosis
- Gallagher, J.C. , Riggs, B.L. & DeLuca, H.F. (1980). Effect of estrogen on calcium absorption and serum vitamin D metabolites in postmenopausal osteoporosis. The Journal of Clinical Endocrinology and Metabolism, 51(6), 1359-1364. http://www.ncbi.nlm.nih.gov/pubmed/6255005
- New York State Department of Health. (2015). Calcium and Healthy Bones. Retrieved May 10, 2016, from https://www.health.ny.gov/publications/1982.pdf
- Office on Women's Health. (2012). Osteoporosis fact sheet. Retrieved May 10, 2016, from http://www.womenshealth.gov/publications/our-publications/fact-sheet/osteoporosis.html
- University of Maryland Medical Center. (2015). Osteoporosis. Retrieved May 10, 2016, from http://umm.edu/health/medical/altmed/condition/osteoporosis
